ICSI vs Conventional IVF: Key Differences Explained
Introduction
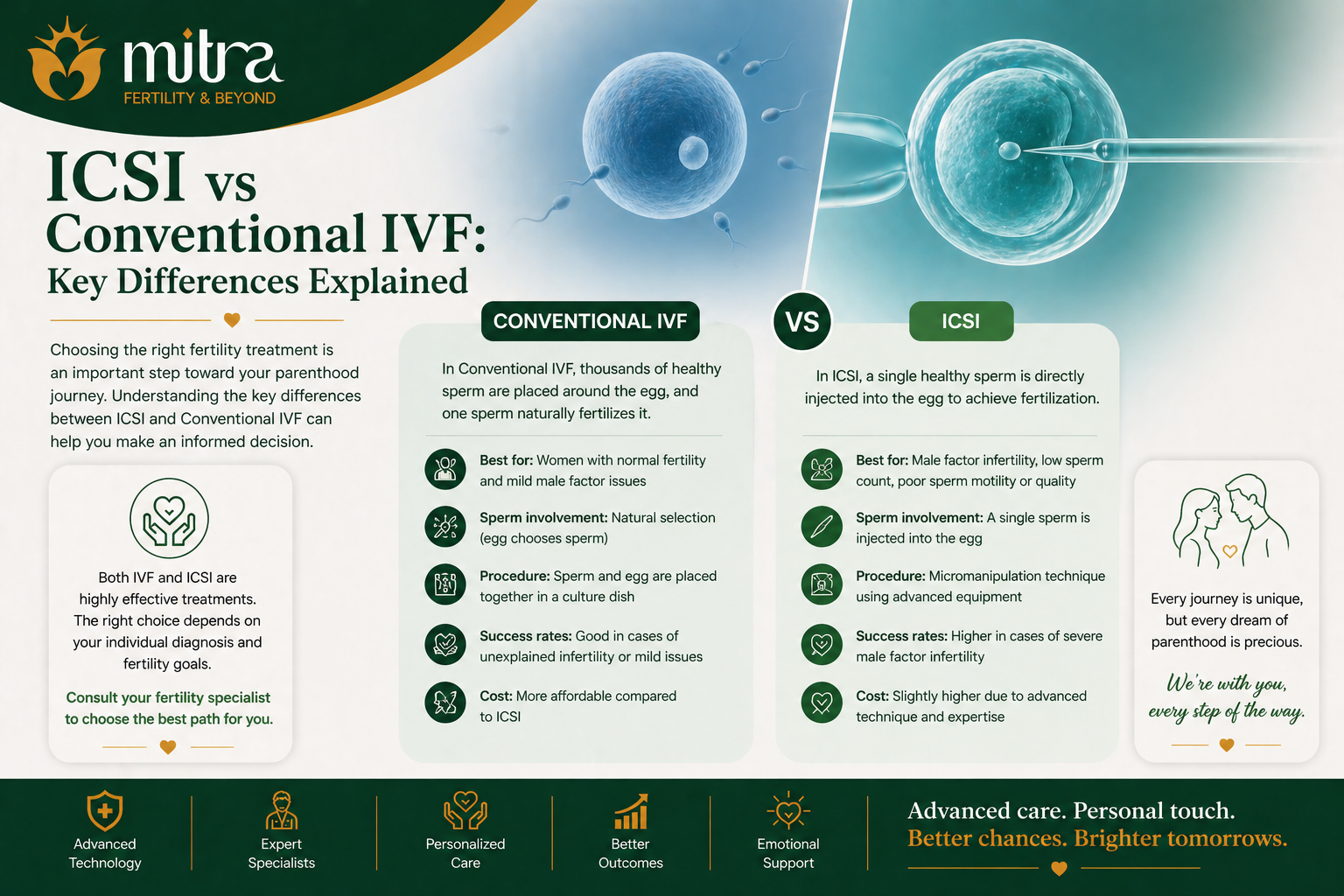
When exploring fertility treatments, many couples come across two commonly used techniques: Conventional IVF and ICSI (Intracytoplasmic Sperm Injection).
While both are part of the IVF process, they differ in how fertilization happens.
Understanding the difference between ICSI vs conventional IVF can help you make informed decisions about your treatment.
What is Conventional IVF?
In conventional IVF:
Eggs are retrieved from the ovaries
Sperm is placed with the eggs in a lab dish
Fertilization occurs naturally, where one sperm enters the egg on its own
Eggs are retrieved from the ovaries
Sperm is placed with the eggs in a lab dish
Fertilization occurs naturally, where one sperm enters the egg on its own
Key point:
Fertilization depends on the sperm’s ability to penetrate the egg naturally.
What is ICSI (Intracytoplasmic Sperm Injection)?
In ICSI:
A single sperm is directly injected into the egg using a specialized technique
A single sperm is directly injected into the egg using a specialized technique
Key point:
Fertilization is assisted, ensuring that sperm enters the egg.
ICSI vs Conventional IVF: Key Differences
Factor
Conventional IVF
ICSI
Fertilization Method
Natural (in lab)
Direct injection
Sperm Requirement
Needs healthy, active sperm
Works even with low-quality sperm
Complexity
Less complex
More advanced technique
Use Case
Normal fertility or mild issues
Severe male infertility
Control Over Fertilization
Limited
High control
Factor | Conventional IVF | ICSI |
Fertilization Method | Natural (in lab) | Direct injection |
Sperm Requirement | Needs healthy, active sperm | Works even with low-quality sperm |
Complexity | Less complex | More advanced technique |
Use Case | Normal fertility or mild issues | Severe male infertility |
Control Over Fertilization | Limited | High control |
When is Conventional IVF Recommended?
Conventional IVF may be suitable when:
Sperm count and motility are normal
No severe male infertility is present
Unexplained infertility cases
It allows fertilization to occur more naturally.
Sperm count and motility are normal
No severe male infertility is present
Unexplained infertility cases
When is ICSI Recommended?
ICSI is typically used in cases of:
Low sperm count
Poor sperm motility
Abnormal sperm shape
Previous IVF fertilization failure
Use of frozen or surgically retrieved sperm
ICSI significantly improves fertilization chances in such cases.
Low sperm count
Poor sperm motility
Abnormal sperm shape
Previous IVF fertilization failure
Use of frozen or surgically retrieved sperm
Success Rates: ICSI vs Conventional IVF
Both methods can achieve similar pregnancy outcomes when used appropriately.
Key insight:
ICSI improves fertilization rates, especially in male infertility cases
Overall pregnancy success depends on:
Embryo quality
Age
Uterine health
ICSI does not necessarily increase success in cases where sperm quality is already normal.
ICSI improves fertilization rates, especially in male infertility cases
Overall pregnancy success depends on:
Embryo quality
Age
Uterine health
Advantages of ICSI
Higher fertilization success in difficult cases
Effective for severe male infertility
Useful in previous IVF failures
Higher fertilization success in difficult cases
Effective for severe male infertility
Useful in previous IVF failures
Advantages of Conventional IVF
Less invasive process for the egg
Mimics natural fertilization
Suitable for cases without sperm-related issues
Less invasive process for the egg
Mimics natural fertilization
Suitable for cases without sperm-related issues
Common Myths About ICSI and IVF
Myth 1: ICSI is Better for Everyone
Fact: It is only beneficial in specific cases.
Myth 2: ICSI Guarantees Pregnancy
Fact: It improves fertilization, not overall pregnancy success.
Myth 3: Conventional IVF is Outdated
Fact: It remains effective for many patients.
Which Option is Right for You?
The choice between ICSI and conventional IVF depends on:
Sperm quality
Fertility history
Previous treatment outcomes
Doctor’s recommendation
There is no universal answer—treatment must be personalized.
Sperm quality
Fertility history
Previous treatment outcomes
Doctor’s recommendation
Conclusion
ICSI and conventional IVF are both effective techniques—but they serve different purposes.
Conventional IVF supports natural fertilization in the lab
ICSI provides a solution when sperm-related challenges exist
Choosing the right method ensures the best possible outcome for your fertility journey.